Oral health is a fundamental component of general health and quality of life, enabling essential functions such as mastication, speech, and social interaction. Dental caries is a biofilm‑mediated, sugar‑driven, multifactorial disease characterized by alternating phases of demineralization and remineralization of the tooth hard tissues. Despite significant global reductions in caries prevalence over recent decades, the disease remains highly prevalent among children and other high‑risk groups. (Rošin-Grget K et al, 2013).
Historically, caries management relied predominantly on surgical removal of diseased tooth structure and placement of restorations. Advances in cariology have shifted this paradigm toward prevention, early diagnosis, and non‑invasive or minimally invasive interventions. Remineralization‑based strategies now form the foundation of modern caries management, focusing on arresting or reversing early lesions rather than restoring cavitated defects.
Fluoride has played a central role in caries prevention due to its ability to inhibit demineralization and enhance remineralization. However, excessive fluoride exposure may lead to adverse outcomes such as dental fluorosis, particularly in young children. Additionally, growing public concern regarding systemic fluoride intake has prompted exploration of effective non‑fluoridated alternatives. This review aims to synthesize current evidence on non‑fluoridated caries preventive agents and technologies, highlighting their mechanisms, clinical effectiveness, and role in contemporary dental practice.
Demineralization- Remineralization Dynamics
Dental caries results from a dynamic imbalance between pathological factors (acidogenic bacteria, fermentable carbohydrates, and reduced salivary flow) and protective factors (saliva, calcium, phosphate, and preventive interventions). (Featherstone JDB 2004). Acid production by cariogenic microorganisms such as Streptococcus mutans lowers plaque pH below the critical threshold (~5.5), resulting in dissolution of hydroxyapatite crystals and subsurface enamel demineralization.
Enamel demineralization initially manifests as non‑cavitated white spot lesions, characterized by increased porosity beneath a relatively intact surface layer. Importantly, this process is reversible. When pH returns to neutral and adequate calcium and phosphate ions are available, remineralization can occur, restoring mineral content and improving enamel resistance to future acid attacks.
Saliva plays a pivotal role in this balance by buffering acids, supplying minerals, and facilitating clearance of carbohydrates and microorganisms. Modern preventive strategies aim to enhance remineralization, stabilize biofilms, and maintain favorable oral environmental conditions to prevent lesion progression. (ten Cate JM 2001)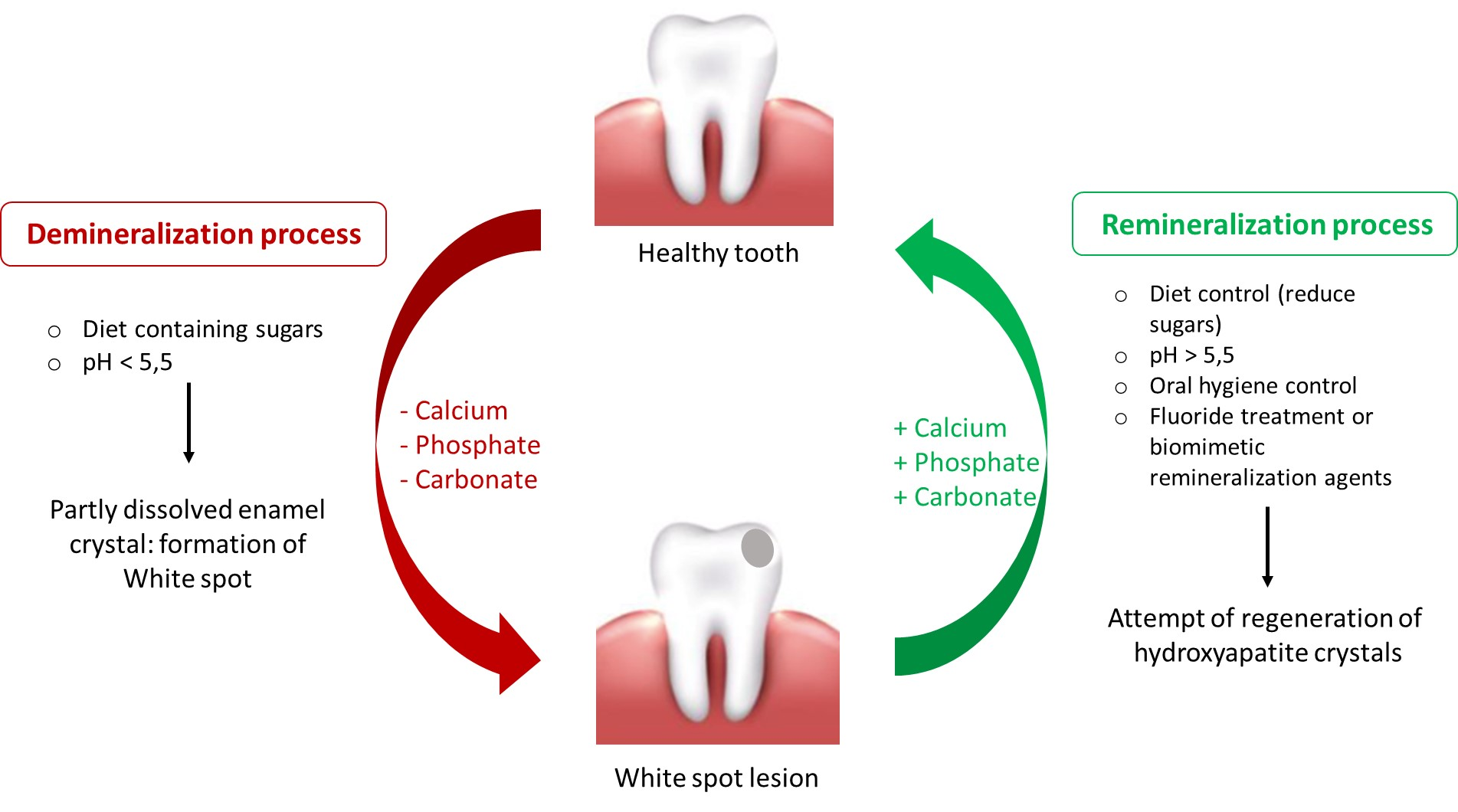
Figure 1: Demineralization and remineralization dynamics
Modern Caries Management Philosphy
The contemporary approach to caries management is guided by the principle of “preserve tooth structure and restore only when necessary.” This philosophy emphasizes risk assessment, early lesion detection, and the use of preventive or micro‑invasive techniques to arrest disease progression. Non‑fluoridated agents support this paradigm by offering safer options for susceptible populations while maintaining efficacy in caries prevention and control. (Schwendicke F, Frencken JE, Bjørndal L, et al. 2016)
Classification of Non-Fluoridated Caries Preventive Agents
Non‑fluoridated caries preventive strategies can be broadly categorized based on their primary mechanism of action:
- Physical barriers – Pit and fissure sealants, resin infiltration
- Mineral enhancers – CPP‑ACP, hydroxyapatite, bioactive glass, theobromine
- Biofilm modifiers – Arginine, xylitol, probiotics
- Antimicrobial agents – Natural and synthetic antimicrobial compounds
PHYSICAL BARRIERS
- Pit and Fissure Sealants
Pit and fissure sealants are resin‑ or glass ionomer‑based materials applied to occlusal pits and fissures of caries‑susceptible teeth, forming a protective barrier that prevents bacterial colonization and nutrient access. Sealants are a cornerstone of preventive dentistry, particularly in children and adolescents. (Simonsen RJ 2002)
Figure 2: Resin sealant placement technique
1.1 Types of Sealants
- Resin‑based sealants: High retention and wear resistance
- Glass ionomer sealants: Fluoride release and moisture tolerance
- Resin‑modified glass ionomer and compomer sealants: Combined advantages of resin and glass ionomer materials
1.2 Clinical Effectiveness
Long‑term studies demonstrate significant reductions in occlusal caries incidence when sealants are properly applied and maintained. Although glass ionomer sealants show lower retention rates compared to resin‑based materials, their caries‑preventive effect may persist due to residual material in fissures and ion release.
- Resin Infilration
Resin infiltration is a micro‑invasive technique designed to arrest non‑cavitated enamel lesions by infiltrating a low‑viscosity resin into the porous lesion body. (Paris S, Meyer-Lueckel H. 2010). The commercially available system (Icon®, DMG) utilizes hydrochloric acid etching, ethanol drying, and resin infiltration to occlude diffusion pathways for acids.
Figure 3: Components of Icon
2.1 Mechanism of Action
The infiltrant penetrates enamel porosities via capillary action, polymerizes within the lesion, and forms a diffusion barrier that inhibits further demineralization. Additionally, resin infiltration improves the optical properties of white spot lesions by matching the refractive index of sound enamel.
2.2 Clinical Applications
- Arrest of early proximal and smooth surface lesions
- Management of post‑orthodontic white spot lesions
- Aesthetic improvement in fluorosis and molar‑incisor hypomineralization
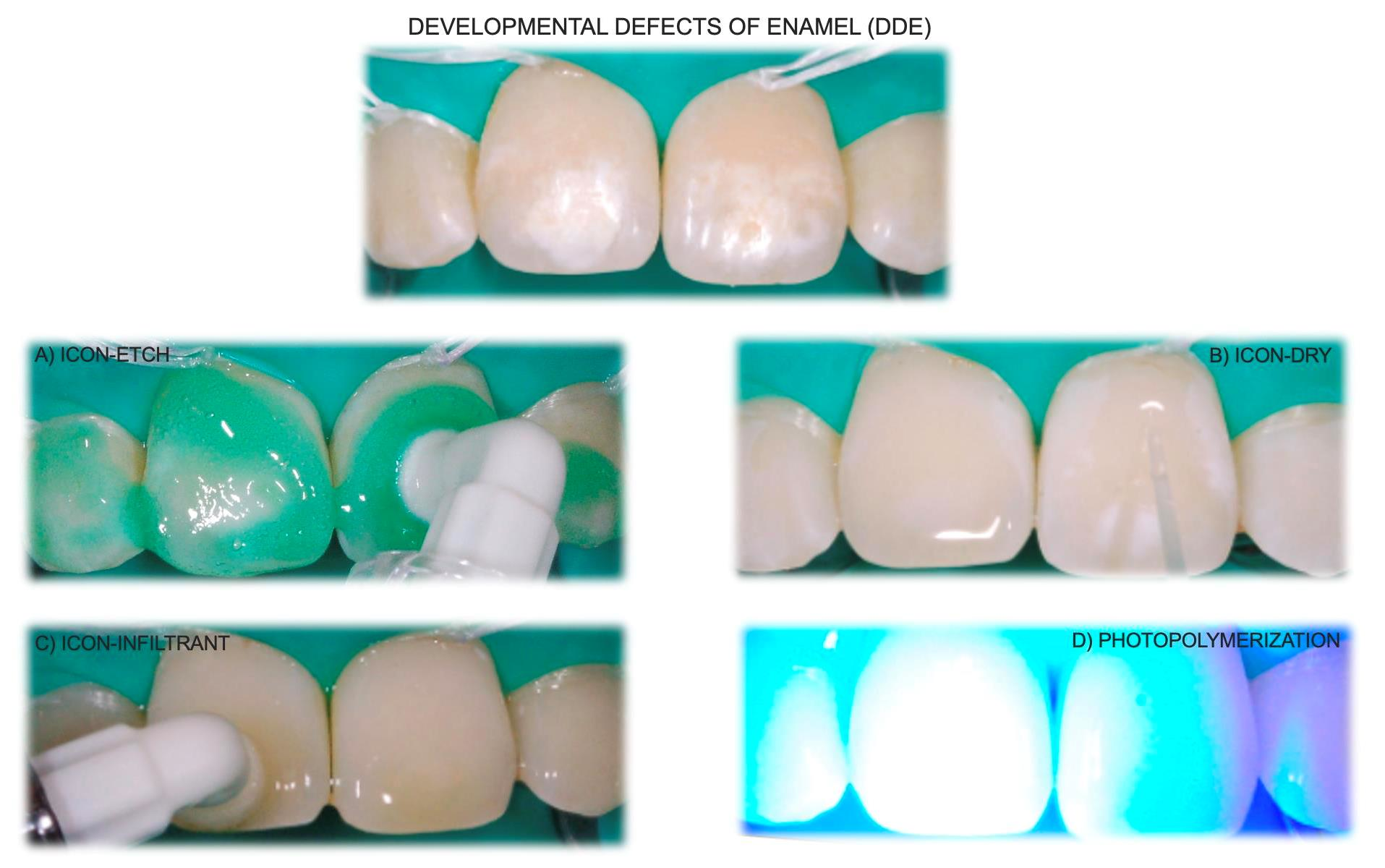 Figure 4: Icon resin infiltration technique
Figure 4: Icon resin infiltration technique
2.3 Limitations
Limited penetration into dentin, potential long‑term discoloration, and technique sensitivity are recognized drawbacks. Ongoing research focuses on enhancing resin formulations with antibacterial and remineralizing components.
MINERAL ENHANCERS
- Casein Phosphopeptide–Amorphous Calcium Phosphate (CPP‑ACP)
CPP‑ACP is a milk‑derived remineralizing agent that stabilizes calcium and phosphate ions in an amorphous, bioavailable form. It acts as a reservoir of minerals within dental plaque and enamel, promoting remineralization and inhibiting demineralization. (Reynolds EC. 1997)
Clinical studies demonstrate its effectiveness in reversing white spot lesions and enhancing enamel resistance, particularly when used as topical creams or chewing gums. (Beerens MW, van der Veen MH, van Beek H, ten Cate JM 2010)
- Hydroxyapatite
Synthetic hydroxyapatite mimics the natural mineral structure of enamel. Nano‑hydroxyapatite particles can penetrate enamel defects, fill micro‑porosities, and promote surface remineralization. Its excellent biocompatibility and absence of toxicity make it suitable for long‑term use. (Amaechi BT AbdulAzees PA, Alshareif DO et al, 2019)
Figure 5: Schematic overview showing the modes of action of HAP in the remineralization and protection of enamel
- Bioactive Glass
Bioactive glass releases calcium, phosphate, and sodium ions in aqueous environments, leading to the formation of a hydroxycarbonate apatite layer on the tooth surface. This process enhances remineralization and provides a protective effect against acid challenges.
Figure 6: Remineralizing characteristics of Bioglass
- Theobromine
Theobromine, a natural alkaloid found in cocoa, has been shown to enhance enamel crystallinity and hardness. It promotes the formation of larger, more acid‑resistant apatite crystals and represents a promising fluoride‑free alternative.
BIOFILM MODIFIERS
- Arginine
Arginine metabolism by arginolytic bacteria produces ammonia, increasing plaque pH and counteracting acidogenic challenges. Arginine‑containing products have demonstrated reduced caries activity and improved plaque ecology.
- Xylitol
Xylitol is a non‑fermentable sugar alcohol that inhibits Streptococcus mutans growth and adhesion. Regular xylitol use enhances salivary flow and reduces cariogenic bacterial load.
(Zero DT. Sugars 2009)
Figure 7: Bi-facet therapeutic efficacy of xylitol on dental caries
- Probiotics
Probiotics aim to restore microbial balance by introducing beneficial bacteria that compete with cariogenic species. Emerging evidence supports their adjunctive role in caries prevention.
ANTIMICROBIAL AGENTS
Natural agents such as propolis, green tea catechins, and essential oils, as well as synthetic agents like chlorhexidine, contribute to caries prevention by reducing microbial load and inhibiting biofilm formation. Their role is primarily adjunctive within comprehensive preventive regimens.
DISCUSSION
Non‑fluoridated caries preventive strategies align well with modern concepts of minimally invasive dentistry. These agents address multiple aspects of the caries process, including mineral loss, biofilm dysbiosis, and surface vulnerability. While fluoride remains highly effective, non‑fluoridated alternatives provide valuable options for individuals at risk of fluorosis, those with specific medical or social considerations, and populations seeking fluoride‑free preventive care
CONCLUSION
A multifaceted strategy is essential for preventing caries in children, typically commencing with appropriate oral hygiene practices such as brushing twice daily and rinsing to eliminate plaque build-up. In addition, managing dietary intake and ensuring regular dental visits can support children in maintaining healthy teeth, fostering a positive relationship with oral hygiene, and preventing the onset of more serious dental issues down the line. Moreover, the use of remineralizing agents in caries prevention represents a significant advancement in modern dentistry. Unlike traditional fluoride methods, non-fluoridated agents work by replenishing essential minerals, such as calcium and phosphate, while also offering alternative approaches to enhance enamel strength and repair microscopic damage. Thus, by integrating these innovative strategies into oral care routines, dentists and researches aim to create a proactive defense system that not only prevents caries but also promotes long-term oral health. (Walsh T, Worthington HV, Glenny AM, et al 2010)
Caries preventive strategies employ a range of mechanisms, among which pit and fissure sealants and resin infiltration are notable for their barrier mechanism. Sealants are applied in the pits and fissures of teeth to inhibit the development of caries, providing essential protection for children with an increased risk of cavities, whereas resin infiltration is commonly used to address early carious lesions on smooth surfaces, particularly white spot lesions on the facial surfaces of anterior teeth. Some compounds utilize a mechanism to elevate mineral saturation, which encompasses CPP-ACP, hydroxyapatite, bioactive glass, and theobromine. These agents provide bioavailable calcium and phosphate ions to demineralized regions, facilitating the restoration of mineral balance and the enhancement of tooth structure integrity. Another approach employed by remineralizing agents involves the alteration of biofilm through pH and microbial modulation. Compounds such as arginine and xylitol function as pH modifiers, creating a more alkaline environment that counteracts the acidogenic activity of cariogenic bacteria, thereby preventing caries. Probiotics, in contrast, play a crucial role in maintaining a balanced oral microbiome by suppressing harmful bacteria and fostering beneficial strains. In addition, agents like chlorhexidine, triclosan, povidone iodine, propolis etc, exhibit antimicrobial properties that can be incorporated into a non-fluoridated prevention plan.
Thus, encouraging awareness and consistency in these practices, not only prevent caries but also enhance children's well-being and self-esteem through a healthier smile.
REFERENCES
- Featherstone JD. The continuum of dental caries—evidence for a dynamic disease process. Journal of dental research. 2004 Jul;83(1_suppl):39-42. ten Cate JM. Remineralization of caries lesions extending into dentin. J Dent Res. 2001;80(5):1407–1411.
- Reynolds E. Remineralization of enamel subsurface lesions by casein phosphopeptide-stabilized calcium phosphate solutions. Journal of dental research. 1997 Sep;76(9):1587-95.
- Paris S, Meyer-Lueckel H. Infiltrants inhibit progression of natural caries lesions in vitro. Journal of dental research. 2010 Nov;89(11):1276-80.
- Simonsen RJ. Pit and fissure sealant: review of the literature. Pediatric dentistry. 2002 Sep;24(5):393-414.
- Amaechi BT, AbdulAzees PA, Alshareif DO, Shehata MA, Lima PP, Abdollahi A, Kalkhorani PS, Evans V. Comparative efficacy of a hydroxyapatite and a fluoride toothpaste for prevention and remineralization of dental caries in children. BDJ open. 2019 Dec 9;5(1):18.
- Schwendicke F, Frencken JE, Bjørndal L, Maltz M, Manton DJ, Ricketts D, Van Landuyt K, Banerjee A, Campus G, Doméjean S, Fontana M. Managing carious lesions: consensus recommendations on carious tissue removal. Advances in dental research. 2016 May;28(2):58-67.
- Zero DT. Sugars–the arch criminal?. Caries research. 2004 May 21;38(3):277-85.
- Philip N. State of the art enamel remineralization systems: the next frontier in caries management. Caries research. 2019 Oct 8;53(3):284-95.
- Beerens MW, van der Veen MH, van Beek H, ten Cate JM. Remineralising effect of MI Paste Plus® on the regression of early caries after orthodontic fixed appliance treatment; a randomized 3-month follow-up clinical trial. White Spot Lesions after Orthodontic Fixed Appliance Treatment The effectiveness of MI Paste Plus® as a remineralising agent a randomised controlled trial. 2010;118(6):55.


 Gursimran Kaur*
Gursimran Kaur*
 Varinder Goyal
Varinder Goyal
 10.5281/zenodo.19881827
10.5281/zenodo.19881827