
We use cookies to ensure our website works properly and to personalise your experience. Cookies policy

We use cookies to ensure our website works properly and to personalise your experience. Cookies policy
TEXILA American University, Lagos, Nigeria
Objective: The objective of this study is to identify medication adherence predictors so that treatments can be personalized to target socioeconomic, psychological, or health system-related issues that could have a detrimental impact on adherence to medication. Methods: Comprehensive search was carried out using databases including African Journals Online (AJOL), PubMed Central, Google Scholar, Science Direct, and JSTOR that contained articles published between 2014 and 2024. Results: The data from the many studies included indicated that access to technology, health-related issues, and demographic characteristics were the main determinants of medication adherence in tuberculosis (TB) patients. Patient-provider interactions were also found to be highly significant in this regard. Furthermore, the effectiveness of e-refill systems in improving treatment results was demonstrated, especially with regard to mobile phone-based interventions, despite challenges such as technical malfunctions and patient accessibility problems in public health facilities. Conclusion: The study highlights the importance of medication adherence in the treatment of tuberculosis and the role various factors, including socio-demographic characteristics and social support, play in patient adherence. To improve treatment outcomes, intervention strategies, such as patient education and healthcare staff training are crucial. Further research should be done on enhancing system efficiency and user diversity to optimize e-refill systems' effectiveness in promoting medication adherence and improving TB treatment outcomes.
Tuberculosis (TB) has been? to be a leading health concern to the global community and its effects are evident in the profound cases of illness and mortality1. Nigeria is included among the countries with the highest burden of TB and thus is faced with the challenges of this contagious disease 2. According to a report by 3 on TB, the incidence rate of TB in the year 2019 was relatively high with about 219 per 100,000 of the population. TB is no more a simple problem given the socio-economic diversity, population density and limited health care facilities across the country.
Such factors as poverty, population density and congestion, inadequate functional health care facilities especially in the rural settings contribute to prevalence of TB burden 4. These factors contribute to diagnostic delays, inadequate treatment, and subsequent challenges in TB control efforts 5. The rise of drug-resistant TB strains further escalates the disease?s severity, necessitating longer and more complicated treatment plans, often with less successful outcomes, thereby posing severe public health threat 6.
The need for improved adherence to TB treatment is a critical factor, influenced by the complex nature of TB therapy and its implications for individual health and public health 7. Therefore, improving medication adherence is a key strategy to reduce the risk of drug resistance and its associated consequences.
The e-Refill system is a significant advancement in healthcare technology, offering a comprehensive approach to improving TB medication adherence 8. The digital nature of the e-Refill system enhances the ease and convenience of medication refills 9.
This review significantly contributes to improving Tuberculosis (TB) treatment outcomes by examining the predictors of medication adherence specifically among TB patients using the e-Refill system and factors influencing adherence in the context of technology-mediated healthcare. This directly contributes to the improvement of TB treatment effectiveness and patient outcomes.
MATERIALS AND METHODS
This systematic review adheres to the SPIDER (Sample, Phenomenon of Interest, Design, Evaluation, and Research) standards for systematic reviews, the approach is planned to be thorough, methodical, and transparent.
SEARCH STRATEGY
?A comprehensive search was conducted to facilitate this research, encompassing publications published from 2014 to 2024, in alignment with the review question. Searches across several databases, was conducted which encompasses a wide range of scholarly publications,?the literature search guarantees a thorough retrieval of pertinent literature. Among these databes are African Journal Online (AJOL), PubMed Central, Google Scholar, Science Direct, and JSTOR. Utilising A thorough search strategy was put into place using a combination of keywords, acronyms, free-text terms, synonyms, wildcards, and transatlantic expressions. The methodological approach chosen was meant to ensure a thorough retrieval of studies that met the predetermined inclusion criteria.
ELIGIBILITY CRITERIA
The inclusion criteria include: (1) Studies that include TB patients who are receiving care through the e-refill prescription system in public healthcare facilities in Lagos. (2) Studies that include the predictors of medication adherence among TB patients. (3) Studies that include patients who can provide information on factors influencing their adherence to TB medication within the context of the e-refill prescription system. The scope of the review was limited to English-only articles to preserve the integrity of the research and reduce any potential difficulties associated with translation.
STUDY SELECTION
The studies were independently reviewed by two researchers. They reviewed each title, abstract, and full text, with any differences resolved through consensus with a third researcher.
Data extraction
Using a predefined extraction form, data was extracted from the included studies. At the end of the data extraction phase, the two researchers again reviewed and did quality check of the extracted data. The extraction for this study comprised of: Author(s), year of publication, title, study objective, geographical location, study setting, methodological information, findings, outcomes and implications. To ensure a methodical gathering of pertinent data from every study incorporated, a standardized data extraction form was developed. The purpose of this form is to collect essential study attributes and results that are consistent with the research objectives.
QUALITY ASSESSMENT
The primary objectives of quality assessment is identifying studies with high methodological quality for inclusion in the review, providing a basis for weighting studies in the synthesis of results, and informing the analysis of the robustness of the review findings. The Critical Appraisal Skills Programme (CASP) Checklists: FOR Qualitative and Quantitative Studies were employed in this research endeavour
DATA ANALYSIS
Subsequently, pertinent information from each study was arranged in order of significance, methodology, primary findings, and objectives. By employing this methodology, the researcher successfully discerned recurring trends and extracted significant revelations from the varied results.
RESULTS AND DISCUSSION
Table 1: Study selection
|
S/N |
Authors and Year |
|
1 |
Tsegahun Manyazewal, Yimtubezinash Woldeamanuel, Tewodros Getinet, Hoover, A., Kidist Bobosha, Oumer Fuad, Getahun, B., Abebaw Fekadu, Holland, D. and Marconi, V.C. (2023). Patient-reported usability and satisfaction with electronic medication event reminder and monitor device for tuberculosis: a multicentre, randomised controlled trial. EClinicalMedicine, 56(Volume 56, February 2023, 101820), pp.101820?101820. doi:https://doi.org/10.1016/j.eclinm.2022.101820. |
|
2 |
Wang, N., Shewade, H.D., Thekkur, P., Huang, F., Yuan, Y., Wang, X., Wang, X., Sun, M. and Zhang, H., 2021. Electronic medication monitor for people with tuberculosis: implementation experience from thirty counties in China. PLoS One, 15(4), p.e0232337. |
|
3 |
Stagg, H., Lewis, J., Liu, X., Huan, S., Jiang, S., Chin, D., & Fielding, K. (2019). Temporal Factors and Missed Doses of Tuberculosis Treatment. A Causal Associations Approach to Analyses of Digital Adherence Data. Annals of the American Thoracic Society, 17, 438 - 449. https://doi.org/10.1513/AnnalsATS.201905-394OC. |
|
4 |
Gashu, K.D., Gelaye, K.A., Lester, R. and Tilahun, B. (2021). Effect of a phone reminder system on patient-centered tuberculosis treatment adherence among adults in Northwest Ethiopia: a randomised controlled trial. BMJ Health & Care Informatics, 28(1), p.e100268. doi:https://doi.org/10.1136/bmjhci-2020-100268. |
|
5 |
Liu, X., Lewis, J.J., Zhang, H., Lu, W., Zhang, S., Zheng, G., Bai, L., Li, J., Li, X., Chen, H., Liu, M., Chen, R., Chi, J., Lu, J., Huan, S., Cheng, S., Wang, L., Jiang, S., Chin, D.P. and Fielding, K.L. (2015). Effectiveness of Electronic Reminders to Improve Medication Adherence in Tuberculosis Patients: A Cluster-Randomised Trial. PLOS Medicine, 12(9), p.e1001876. doi:https://doi.org/10.1371/journal.pmed.1001876. |
|
6 |
Wang, N., Guo, L., Shewade, H. D., Thekkur, P., Zhang, H., Yuan, Y.-L., Wang, X.-M., Wang, X.-L., Sun, M.-M., Huang, F., & Zhao, Y.-L. (2021). Effect of using electronic medication monitors on tuberculosis treatment outcomes in China: a longitudinal ecological study. Infectious Diseases of Poverty, 10(1). https://doi.org/10.1186/s40249-021-00818-3 |
|
7 |
Wang, X., Fu, Q., Zhou, M., & Li, Y. (2024). How Integrated Digital Tools Can Improve Tuberculosis Medication Adherence: A Longitudinal Study in China. Telemedicine Journal and E-Health. https://doi.org/10.1089/tmj.2023.0084 |
|
8 |
Maro, R. A, Mtenga, A., Benson Mtesha, Wilhelm, K., Emmanuel, N., Marion Sumari-de Boer, & Kennedy Ngowi. (2024). Implementation bottlenecks of real time medication monitoring (evriMED) for improving adherence to anti-TB drugs among people with tuberculosis in Kilimanjaro, Tanzania. Journal of Clinical Tuberculosis and Other Mycobacterial Diseases, 34, 100409?100409. https://doi.org/10.1016/j.jctube.2023.100409 |
|
9 |
?Du, L., Chen, X., Zhu, X., Zhang, Y., Wu, R., Xu, J., ? Lu, X. (2020). Determinants of Medication Adherence for Pulmonary Tuberculosis Patients During Continuation Phase in Dalian, Northeast China. Patient Preference and Adherence, Volume 14, 1119?1128. https://doi.org/10.2147/ppa.s243734 |
|
10 |
Panicker, R. O., & Sabu, M. K. (2019). Factors influencing the adoption of computerized medical diagnosing system for tuberculosis. International Journal of Information Technology. https://doi.org/10.1007/s41870-019-00396-6 |
|
11 |
Mohammed, S., Glennerster, R., & Khan, A. J. (2016). Impact of a Daily SMS Medication Reminder System on Tuberculosis Treatment Outcomes: A Randomized Controlled Trial. PLOS ONE, 11(11), e0162944. https://doi.org/10.1371/journal.pone.0162944 |
|
12 |
Born, A. L. (2016).?Patients' perceptions of pharmacy services?(Doctoral dissertation, University of Toledo). |
|
13 |
Zhang, M., Wang, G., Najmi, H., Yaqoob, A., Li, T., Xia, Y., ? Li, Y. (2023). Digitizing tuberculosis treatment monitoring in Wuhan city, China, 2020-2021: Impact on medication adherence. Frontiers in Public Health, 11, 1033532. https://doi.org/10.3389/fpubh.2023.1033532 |
|
14 |
Sazali, M. F., Rahim, S. S. S. A., Mohammad, A. H., Kadir, F., Payus, A. O., Avoi, R., ... & Azhar, Z. I. (2023). Improving Tuberculosis Medication Adherence: The Potential of Integrating Digital Technology and Health Belief Model.?Tuberculosis and respiratory diseases,?86(2), 82. |
|
15 |
Siti Aishah Abas, Ismail, N., Zakaria, Y., Siti Munira Yasin, Ibrahim, K. A., Ismail, I., ? Ahmad, N. (2024). Enhancing tuberculosis treatment adherence and motivation through gamified real-time mobile app utilization: a single-arm intervention study. BMC Public Health, 24(1). https://doi.org/10.1186/s12889-023-17561-z |
|
16 |
Lester, R., Park, J. J., Bolten, L. M., Enjetti, A., Johnston, J. C., Schwartzman, K., ? Delft, A. von. (2019). Mobile phone short message service for adherence support and care of patients with tuberculosis infection: Evidence and opportunity. Journal of Clinical Tuberculosis and Other Mycobacterial Diseases, 16, 100108. https://doi.org/10.1016/j.jctube.2019.100108 |
|
17 |
Fang, X. H., Guan, S. Y., Tang, L., Tao, F. B., Zou, Z., Wang, J. X., ... & Pan, H. F. (2017). Effect of short message service on management of pulmonary tuberculosis patients in Anhui Province, China: a prospective, randomized, controlled study.?Medical science monitor: international medical journal of experimental and clinical research,?23, 2465. |
|
18 |
Story, A., Garfein, R. S., Hayward, A., Rusovich, V., Dadu, A., Soltan, V., ... & Falzon, D. (2016). Monitoring therapy adherence of tuberculosis patients by using video-enabled electronic devices.?Emerging infectious diseases,?22(3), 538. |
|
19 |
Boutilier, J. J., Yoeli, E., Rathauser, J., Owiti, P., Subbaraman, R., & J?nasson, J. O. (2022). Can digital adherence technologies reduce inequity in tuberculosis treatment success? Evidence from a randomised controlled trial. BMJ Global Health, 7(12), e010512. https://doi.org/10.1136/bmjgh-2022-010512 |
|
20 |
Cattamanchi, A., Crowder, R., Kityamuwesi, A., Kiwanuka, N., Lamunu, M., Namale, C., ... & Katamba, A. (2021). Digital adherence technology for tuberculosis treatment supervision: A stepped-wedge cluster-randomized trial in Uganda.?PLoS medicine,?18(5), e1003628 |
|
21 |
Saunders, M., Wingfield, T., Tovar, M. A., Herlihy, N., Rocha, C. M., Zevallos, K., ? Evans, C. A. (2018). Mobile phone interventions for tuberculosis should ensure access to mobile phones to enhance equity - a prospective, observational cohort study in Peruvian shantytowns. 23(8), 850?859. https://doi.org/10.1111/tmi.13087 |
|
22 |
Thomas, B. E., Kumar, J. V., Onongaya, C., Bhatt, S. N., Galivanche, A., Periyasamy, M., ? Subbaraman, R. (2020). Explaining Differences in the Acceptability of 99DOTS, a Cell Phone?Based Strategy for Monitoring Adherence to Tuberculosis Medications: Qualitative Study of Patients and Health Care Providers. JMIR MHealth and UHealth, 8(7), e16634. https://doi.org/10.2196/16634 |
? ? ? ?
? ? ? ? ? ? 
? ? ? ?
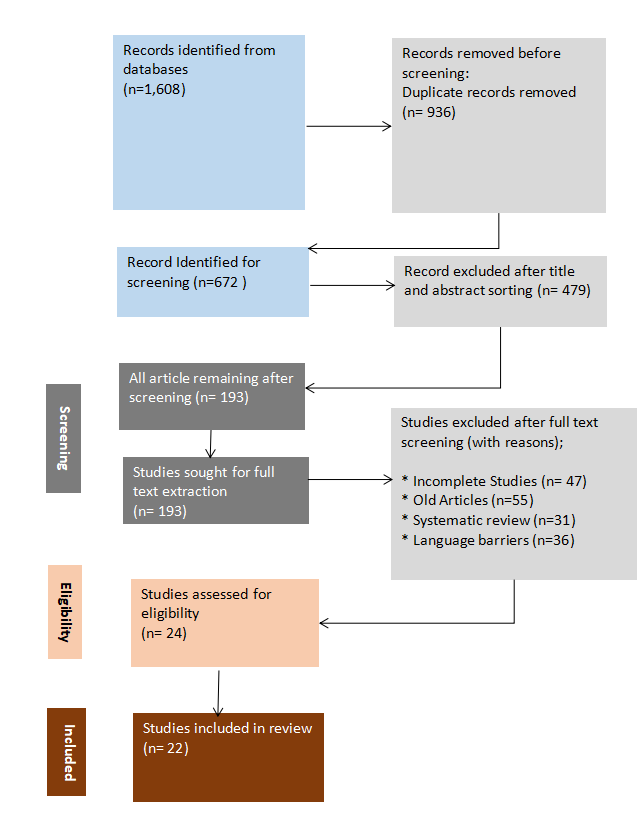
Figure 1:??? Prisma Flow Chat
Table 2: Table of Study Characteristics
|
S/N |
Author & Date |
Objectives??????????????? |
Methodology |
Findings??????????????? |
Conclusion |
|
1. |
Tsegahun Manyazewal et al, 2023 |
This research aimed to evaluate treatment satisfaction and the usefulness of a digital medication event reminder and monitor (MERM) device in patients with tuberculosis, thereby addressing the secondary goal of the SELFTB trial. |
The study employed a multicenter, randomised controlled trial design in Ethiopia, recruiting individuals with advanced pulmonary tuberculosis.? A 15-day medication supply with the MERM device or standard in-person directly observed therapy (DOT) was given to randomly selected participants. Usability was assessed using the Adapted System Usability Scale (SUS), and treatment satisfaction was measured using the Treatment Satisfaction Questionnaire for Medication, version 4 (TSQM 1.4?). |
The MERM device's usability was excellent, with a high likelihood of recommendation by users; however, there was no significant association between usability and medication adherence. Remarkably higher treatment satisfaction scores were found in the intervention group across effectiveness, convenience, and global satisfaction domains. ? |
The study suggests that digital adherence technology, such as the MERM device, can enhance treatment satisfaction among tuberculosis patients, with excellent usability, potentially transforming patient-centered care in high tuberculosis burden countries. |
|
2. |
Wang et al., 2021 |
We assessed the i) proportion eligible for using EMM, ii) uptake of EMM and factors associated, and iii) treatment adherence, including the proportion shifted to DOT, among people with tuberculosis notified in 30 counties in China (July-December 2018), where EMM supported self-administered treatment was suggested to all those eligible (no communication impairment, ambulatory care). |
This study was observational and employed secondary program data. To move to DOT, a single incident of ?50% or a continuous instance of 20?49% monthly missing doses was required. To investigate factors related with not utilizing EMM within the first month, we used log binomial regression. ? |
1810 (81%) of the 2227 people whose EMM eligibility data were available were eligible for EMM. Of them, 1314 (73%) had ever used EMM at some point during their therapy; of them, 10% were shifted to DOT based on EMM data, and 22% were shifted. Furthermore, 70 people were moved during the period when EMM data was unavailable. In the first month of utilising EMM, 25% of users encountered missing EMM data. Age, employment status, tuberculosis type, and history of previous treatment were factors connected with non-use of EMM within the first month. ? |
The study found satisfactory uptake of EMM, but highlighted the need to ensure shift to DOT based on adherence data from EMM. It also emphasized the necessity for clarification in guidelines regarding subsequent follow-up actions when EMM data is missing. |
|
3. |
Stagg et al, 2019 |
To provide specific details about how patients take their medicine for tuberculosis and the time periods connected to missing doses ? |
This study comprised pulmonary tuberculosis patients who were part of a cluster-randomized, pragmatic trial in China that tested the use of electronic reminders to enhance treatment compliance. ?Adherence?to medication without reminders were tracked using medication monitor boxes?(box?openings). We discussed and illustrated the adherence patterns. Ninety doses were given every other day over the typical six-month course of treatment (180 days). To investigate the temporal factors related to the adoption of per-dose suboptimal dosing, taking into consideration participant clustering, mixed-effects logistic regression models were employed. The relationship between early administration of inadequate dosage and permanent discontinuance was investigated using Cox regression models. |
Results showed that 23.9% of doses were missed, and that inadequate dosage implementation was responsible for 56.5% of missing doses. At 60 days, 5.1% of participants had stopped, and at 120 days, that number had increased to 14.4%. Although 22.6% had intervals of two weeks or longer, the majority of subjects (95.9%) missed at least one dosage, mostly single-dose gaps (71.4%). According to adjusted models, there was a higher likelihood of inadequate dosage implementation during the initiation-continuation phase transition and during national holidays. Higher dropout rates were connected with early introduction of inadequate dosage. |
digital tools offer significant advancements in understanding and addressing nonadherence. The study highlighted common nonadherence among tuberculosis patients and the complexity of adherence patterns. It identified increasing rates of both suboptimal dosing implementation and discontinuation over time, with early suboptimal dosing implementation linked to higher discontinuation rates. These findings suggest opportunities for targeted interventions based on temporal factors influencing nonadherence. Top of Form ? |
|
4. |
Gashu et al, 2021 |
The purpose of this research is to determine whether a phone reminder system can improve patient-centered TB treatment adherence in the continuation phase, when patients are in charge of taking their own medications at home. ? |
During the continuation phase, adult TB patients were the subjects of a two-arm randomised controlled trial conducted by the study. In addition to routine care, patients in the intervention group received?refills for drugs every week and daily medication reminders via phone. The control group's members just received routine medical care. Covariate adaptive randomisation was used to balance the variables during allocation. The primary goal was adherence to patient-centered TB treatment; secondary outcomes were treatment outcomes and the patient-physician relationship. Intention-to-treat and per-protocol analytic techniques were applied. ? |
306 patients were randomly assigned, 152 to the intervention?group and 154 to the control group, according to the findings. Relative risk of 1.632 (p=0.018, one-tailed) indicated that the intervention group's adherence to patient-centered TB treatment was considerably higher (79%) than that of the control group (66.4%). Additionally, the intervention group (73.3%) had a considerably higher prevalence of positive provider-patient relationships than the control group (52.4%). The two groups' rates of TB treatment success (89.5% in the intervention group vs. 85.1% in the control group, p=0.1238) did not differ significantly. |
The patient-provider connection and adherence to patient-centered TB therapy were enhanced by a weekly refilling system that combined a daily medication reminder with a mobile phone; treatment success was not significantly affected. ? |
|
5. |
Liu et al, 2015 |
The purpose of the study was to evaluate the effectiveness of medication monitors and text messaging on tuberculosis (TB) patients' medication adherence. ? |
A pragmatic cluster-randomized trial involving patients with active pulmonary tuberculosis was done by the study in 36 districts/counties in China. Text messages, medication monitors, combination intervention, or control were the four case-management strategies that patients were randomly assigned to. The recommendations for more intensive management or directly observed treatment (DOT) for patients with adherence concerns included reminders for medication ingestion and monthly follow-up visits. Reminders were included in the medication monitor and combination arms, and patients used medication monitor boxes to record when the box was opened. |
According?to?the?findings, the medication monitor arm (17.0%) had the lowest number of patient-months with at least 20% of doses missed among the 4,292 recruited TB patients, . This was followed by the text message arm (27.3%), combined arm (13.9%), and control arm (29.9%). The text messaging arm had a lower patient loss to follow-up than the control arm did. All study arms reported equipment malfunctions or operation mistakes, although dividing the patient population into groups with and without drug monitor issues did not change the findings. Intense management was not fully utilised from the beginning. |
To the best of our knowledge, this is the first study to show how a medication monitor can enhance TB patients' medication adherence using a randomised trial design. Medication monitor reminders, but not text message reminders, improved medication adherence in tuberculosis patients. These kinds of innovative strategies for encouraging patients to complete their TB treatment are essential in a country like China where the broad use of DOT is not feasible. ? |
|
6. |
Wang et al, 2021 |
The purpose of the study is to evaluate how using electronic medication monitors (EMMs) has affected the results of tuberculosis (TB) treatment in 138 counties spread over three Chinese provinces. |
Using aggregate secondary programmatic data, the longitudinal ecological technique was used at the county level. This analysis covered all notified cases of TB in 138 counties between April 2017 and June 2019, excluding those that were resistant to rifampicin. A multilevel model measuring the relative change in the quarterly treatment success rate with increasing quarterly EMM coverage rate was fitted, and we took into account seasonal trends, population size, sociodemographic and clinical features, and clustering within counties. A random intercept mixed effects maximum likelihood regression was employed in the model. ? |
Following the implementation of EMMs, the treatment success rate for 69,678 notified TB cases increased marginally from 93.5% to 94.9% in the second quarters of 2018 and 2019. A 10% increase in EMM coverage was linked to a 0.2% increase in treatment success rate, indicating a statistically significant correlation between quarterly EMM coverage and treatment success rate (p = 0.0036). A lower treatment success rate was also linked to variables like an increase in the elderly or TB cases with bacteriological confirmation. |
A statistically significant relationship was seen between the treatment success rate at the county level and the extent of EMM coverage under programming conditions. To verify how employing EMM affects TB treatment outcomes, more prospective trials are required. Future work on EMMs that offer real-time data under programming conditions should be conducted by us, we advise. ? |
|
7. |
Wang et al, 2024 |
The study aimed to evaluate the effectiveness of an integrated digital adherence intervention for tuberculosis (TB) patients, addressing poor medication adherence through a comprehensive approach. |
Electronic medication monitors (EMMs), manual reminders, and instant?WeChat messaging were all integrated into a digital adherence intervention platform. The platform aimed to increase treatment adherence and improve accessibility to digital adherence technology. Enrolled were newly diagnosed tuberculosis patients from January to June 2022 at 10 hospitals with a tuberculosis designation located in 220 communities. We examined fundamental characteristics and treatment compliance of patients in the traditional, EMM, and WeChat groups. To find the factors promoting high medication adherence, a logistic regression analysis was performed. |
A grand total of 2,494 tuberculosis patients were recruited; of these, 14.5% were treated with digital technologies, 9.5% with WeChat, and 5.0% with EMM. Following the intervention, the median medication rates of the patients in the WeChat and EMM groups were significantly higher?95.3% and 95.7%, respectively?than in the conventional group (83.8%). The WeChat and EMM groups, on the other hand, had a substantially lower median number of missed prescriptions than the conventional group. WeChat and EMM groups had higher proportions of high adherence (adherence medication rate ?90%) than the conventional group did. |
The integrated digital adherence intervention technology could be used to help TB patients adhere to their drug regimens more closely. Complementary technologies could be used in practice to increase the accessibility of digital adherence technology. |
|
8. |
Maro et al, 2024 |
In this study, TB patients and directly observed treatment (DOT) nurses were required to identify implementation constraints related to real-time monitoring of medications using the evriMED device. |
A mixed-methods approach was employed, involving TB patients and DOT nurses who participated in the REMIND-TB trial utilizing the evriMED devices. The evriMED device is a medication dispenser with internet connectivity that sends real-time SMS reminders. Data were gathered from the Wisepill dashboard, documenting device activity status. In-depth interviews with TB patients and DOT nurses were conducted using the Measurement Instrument for Determinants of Innovation (MIDI) to identify factors influencing evriMED implementation. |
Out of 281 participants initially given devices, 245 completed the 6-month follow-up period. At month 6, most devices (49%) reported battery-related challenges, and 14% reported more than one incidence of communication loss. TB patients perceived evriMED as user-friendly, facilitating improved medication intake. DOT nurses also saw it as a relevant tool for TB patients but identified implementation bottlenecks such as network issues, limited training, and low technological knowledge among DOT nurses, which led to communication loss. |
The implementation of evriMED was perceived positively by TB patients, enhancing medication intake. However, several implementation bottlenecks were identified, including network issues, limited training, and low technological knowledge among DOT nurses. Addressing these challenges is crucial to successfully implement evriMED as a tool for improving medication adherence among TB patients. Further research is recommended to develop effective strategies to overcome these limitations. |
|
9. |
Du et al, 2020 |
The purpose of the study was to investigate the degree of medication adherence among outpatients with pulmonary tuberculosis in northeast China and to use the bio-psycho-social medical model to uncover predictive factors. ? |
A cross-sectional multi-center survey was conducted in four tuberculosis medical institutions in Dalian, northeast China. Medication adherence was assessed using the eight-item Chinese version of the Morisky Medication Adherence Scale, which divides compliance into three stages. TB knowledge, treatment factors, sociodemographic traits, mental health, and behavioral traits were all regarded as independent variables. Using Stata/MP 14.0, multivariate ordinal logistic regression, the chi-square test, and descriptive statistics were used in the data analysis. ? |
Among 564 eligible participants, 41.84% exhibited high medication adherence, 32.45% medium adherence, and 25.71% low adherence. Multivariate ordinal logistic regression revealed several factors associated with medication adherence. Older age, employment, better TB knowledge, and abstaining from alcohol correlated with higher adherence. Conversely, not following doctors' advice on adjuvant drugs, previous TB treatment, adverse drug reactions, stigma experiences, and requiring supervised treatment were associated with lower adherence. |
Medication adherence among tuberculosis patients in northeast China was influenced by various factors encompassing sociodemographic characteristics, treatment factors, TB knowledge, mental health, and behavioral characteristics. The findings underscore the multifaceted nature of medication adherence in this population. |
|
10. |
Panicker & Sabu, 2019 |
This research aimed to examine the factors influencing the adoption of a Computer-assisted Medical Diagnosing system for Tuberculosis by clinicians and lab technicians in developing countries' healthcare settings. |
A qualitative approach was employed, conducting indepth interviews with clinicians and lab technicians. A total of 18 interviews were conducted, and the collected data were analyzed using content analysis. |
The results revealed several factors influencing the adoption of the CMD system for TB. These factors included human characteristics such as age and computer knowledge, technological characteristics such as performance expectancy and effort expectancy, organizational characteristics such as training and support, and technological impact. |
The study highlighted the importance of understanding various factors that influence the adoption of technological innovations in healthcare settings. The findings provide insights for researchers and medical professionals, enhancing their understanding of technological adoption and assisting in determining the uptake of recent technology by healthcare professionals. |
|
11. |
Mohammed et al, 2016 |
The study aimed to measure the impact of Zindagi SMS, a two-way SMS reminder system, on the treatment success of individuals with drug-sensitive tuberculosis in Karachi, Pakistan. |
A two-arm, parallel design, effectiveness randomized controlled trial was conducted. Individual participants were randomly assigned to either the Zindagi SMS group or the control group. Zindagi SMS sent daily SMS reminders to participants and prompted them to respond through SMS or missed (unbilled) calls after taking their medication. Non-respondents received up to three reminders per day. The trial was conducted in public and public sector tuberculosis clinics in Karachi, Pakistan. |
The study enrolled 2,207 newly-diagnosed patients with smear or bacteriologically positive pulmonary tuberculosis. Among them, 1,110 were randomized to the Zindagi SMS group and 1,097 to the control group. The primary outcome, clinically recorded treatment success based on intention-to-treat, did not show a significant difference between the Zindagi SMS group and the control group (83% vs. 83%, respectively, p = 0.782). Moreover, there was no significant program effect on self-reported medication adherence during unannounced visits throughout treatment. |
Despite its large-scale implementation, the study found no significant impact of SMS medication reminders on tuberculosis treatment outcomes. |
|
12. |
Born, 2016 |
The study aimed to determine the factors influencing patients' perceived benefits of various pharmacy services, including adherence packaging, medication therapy management (MTM), delivery, automatic refill, and refill synchronization. Additionally, it sought to identify the perceived benefits that predict patients' interest in participating in these pharmacy services. |
A cross-sectional exploratory study was conducted using convenience sampling over a seven-week period. Survey questions were developed through elicitation interviews, and validity and reliability were assessed using factor analysis and Cronbach's alpha, respectively. Linear regression and logistic regression analyses were performed. |
A total of 304 surveys were collected, revealing that the majority of participants were unaware of refill synchronization (68.4%), MTM (58.2%), and adherence packaging (77.3%). Age and the number of medications were significant factors influencing how patients perceived the benefits of pharmacy services. Participants who believed that adherence packaging, MTM, delivery, automatic refill, and refill synchronization would help them feel more in control of taking their medication were more likely to participate in these services. |
The study underscores the importance of assessing patients' perceptions to enhance their participation in pharmacy services. Pharmacies should tailor their services to address patients' beliefs and perceived benefits to increase patient engagement and adherence. |
|
13. |
Zhang, 2023 |
The study aimed to investigate the impact of digitizing tuberculosis (TB) treatment monitoring on adherence among TB patients in Wuhan, China, during 2020-2021. |
A cross-sectional study design was employed, comparing an electronic system (e-Patient Service System; e-PSS) introduced for TB medication adherence monitoring with the paper-based standard of care (TB Control Information System; TCIS). Retrospective data for drug-susceptible pulmonary TB patients recorded on both systems were analyzed. Key indicators included compliance with the first follow-up visit, medication adherence (defined as 80% or more of monthly doses taken), and treatment success after six months of follow-up. |
A total of 1,576 TB patients were recorded in TCIS from July to September 2020, while 1,145 TB cases were included in e-PSS from January to March 2021. Demographic and clinical features were similar between the two groups. Patients in the e-PSS group exhibited a higher proportion of visits to community doctors within the first three days compared to the TCIS group. Medication adherence over the 6-month treatment period was also higher in the e-PSS group compared to the TCIS group. Treatment success rates were similar between the two groups. Multivariate logistic regression analysis indicated adjusted odds ratios favoring the e-PSS group for compliant first follow-up visit and medication adherence, though no significant difference was observed in treatment outcome between the two groups. |
The study demonstrated improvements in TB care with the implementation of a digital monitoring intervention in Wuhan, China. |
|
14. |
Sazali, 2023 |
The study aimed to review the latest evidence regarding tuberculosis (TB) medication non-adherence, its associated factors, the efficacy of directly observed therapy (DOT) and its alternatives, and the utilization of digital technology and the health belief model (HBM) in improving medication adherence for TB treatment. |
A narrative review methodology was employed to analyze related articles and address the study objectives. |
The review highlighted the significant public health concern posed by TB and its impact as a leading cause of death globally. Non-adherence to TB therapy was identified as a crucial issue affecting clinical and public health outcomes. While DOT has been introduced as a standard strategy to improve medication adherence, it has faced criticism due to various challenges, including inconvenience, stigma, and reduced quality of life. The effectiveness of DOT in improving anti-TB adherence is also debatable. Therefore, digital technology emerges as a potential tool to enhance DOT implementation and improve medication adherence. Integrating the health belief model (HBM) into digital technology development was identified as potentially effective in changing behavior and enhancing medication adherence for TB treatment. |
Conventional DOT has limitations in TB management, and integrating the health belief model into digital technology offers promise in addressing medication adherence challenges. Digital technology provides an opportunity to overcome various issues related to DOT implementation and improve medication adherence for TB treatment. |
|
15. |
Siti Aishah Abas, 2024 |
The study aimed to determine the impact of Gamified Real-time Video Observed Therapy (GRVOTS) mobile apps on patient medication adherence rates and motivation among tuberculosis (TB) patients in Malaysia. |
A single-arm intervention study was conducted involving 71 patients from 18 healthcare facilities over an 8-week period. Participants were provided with GRVOTS mobile apps and instructed to fulfill tasks such as providing Video Direct Observe Therapy (VDOTS) daily and reporting side effects. Data on VDOT adherence, medication adherence assessed by the Malaysian Medication Adherence Assessment Tool (MyMAAT), and motivation assessed by the Intrinsic Motivation Inventory (IMI) questionnaire were collected at three time intervals: baseline, 1-month, and 2-month intervals. Statistical analysis included one-sample t-test to compare VDOT video adherence to the standard rate of 80%, and repeated measures ANOVA to analyze changes in MyMAAT and IMI scores across the three time intervals. |
The study revealed a significantly higher treatment adherence score of 90.87% among participants, compared to the standard rate of 80%. Participants' MyMAAT and IMI scores also showed significant increases over the three time intervals, with the IMI Interes
Akinremi-Aina Titilope*, Dangana Jonathan, The Predictors of Medication Adherence Among Tb Patients on the E-Refill Prescription System in Health Care Facilities in Lagos ? A Systematic Review, Int. J. Sci. R. Tech., 2024, 1 (11), 28-50. https://doi.org/10.5281/zenodo.14160245 |